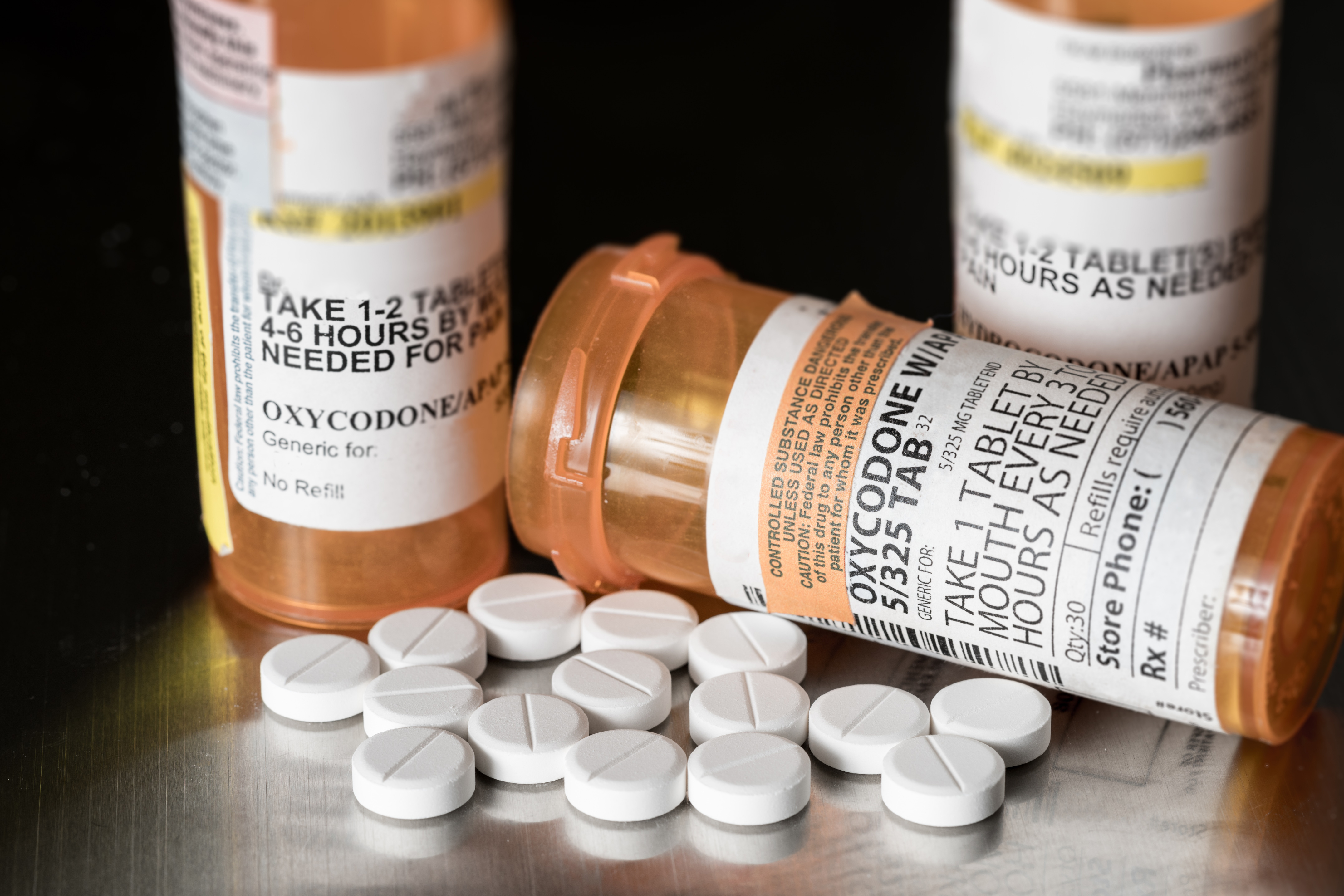
Opiate addiction continues to be a health concern across the country, state, and in the Flathead Valley, though local providers say education about this family of drugs has led to better awareness of its addictive properties.
On Dec. 4, Montana Attorney General Tim Fox filed a lawsuit on behalf of the state against Purdue Pharma LLC, the pharmaceutical behemoth responsible for a host of prescriptions opiates, including OxyContin.
Fox alleges that the company used deceptive marketing practices to make untrue claims about OxyContin and addictive properties.
“Pharmaceutical companies that knowingly and deceptively harm consumers must be held accountable,” Fox stated. “As our investigation revealed and our complaint alleges, for years, Purdue knew the damage caused by OxyContin, and rather than scale back or eliminate distribution of the drug, it ramped-up deceptive marketing tactics to present the drug as ‘safe.’ Purdue manipulates doctors, lies to consumers, and its actions contributed to thousands of deaths across the country.”
Opiate addiction is entrenched across the United States; over the last 18 years, overdose deaths involving opiates have nearly quadrupled. According to the U.S. Department of Health and Human Services, 64,000 people died from overdoses in 2016, and the national Centers for Disease Control and Prevention reports that of the 140 Americans who die from drug overdoses every day, 91 are due to opioids.
In Montana, more than 700 people have died from opiate overdose since 2000, according to the Department of Justice.
Across the Flathead Valley, education about opiates and the understanding of their addictive nature seems to be taking root, according to medical professionals.
Michael Cummins, executive director at the Flathead Valley Chemical Dependency Center, said the number of people seeking treatment for opiate addiction is increasing here, but not as drastically as in other states.
The bulk of the center’s clients are there to primarily treat addiction to alcohol (61.7 percent), followed by meth (17 percent), then marijuana (11.5 percent). Opiates clock in at about 6.8 percent of primary addictions.
The same was true for secondary addictions; marijuana ranked highest at 39.5 percent, followed by alcohol at 19 percent, then meth at 10.3 percent, and finally opiates at 8 percent.
“Within the opiate family, where we’ve seen the biggest uptick within that grouping is heroin,” Cummins said. “A lot of times people will have access to prescription medications either legally or illegally and that either dries up or it becomes too costly. Heroin is cheaper.”
Medical providers are also more wary of prescribing opiates for chronic pain, according to Dr. Jason Cohen, chief medical officer and hospitalist at North Valley Hospital.
“Physicians are just a lot more hesitant now to prescribe opiate medication, the awareness of the addictive properties is better understood by practitioners and the risks associated with them,” Cohen said.
In spring 2016, the CDC issued new opioid prescription guidelines for doctors in an attempt to address the national epidemic. In response, many providers simply decided to stop prescribing opiates, and patients funneled to doctors who would.
Partly in response to prescription fears and partly because of a better understanding about the drugs, physicians and administrators at both North Valley and Kalispell Regional Medical Center are building a common, chronic-opioid policy, Cohen said.
This means a standardized, consistent process of prescribing opiates, not only so patients and providers are on the same page about the drugs, but also so providers can find relief in knowing everyone is prescribing it the same way across the valley.
“It would also include a patient-provider understanding that goes through how it’ll be prescribed and how it shouldn’t be used, setting up clear expectations for both and talking about all the risks,” Cohen said.
Education continues to be one of the most important tools used to battle opiate addiction, including for providers about more modalities of therapy to use for pain relief. But more and more, people are aware of the inherent risks of opiates, he said.
“As a hospitalist, I increasingly encounter more patients who say, ‘I don’t want any opiates, I don’t want to get addicted,'” Cohen said.
Cohen said there’s not a specific type of person who ends up addicted.
“I think there’s a lot of judgment out there about chronic-opiate use,” Cohen said. “As a provider I can tell you this isn’t just one neighborhood or group of people. It’s pretty rare that someone doesn’t know someone with a problem.”