Marketplace Enrollment Numbers See Initial Drop in Montana
The state saw about a 6% decrease, marking the first time enrollment has gone down since 2020. The full impact of expiring enhanced ACA tax credits is anticipated to come after enrollees have paid their premiums.
By Zoë Buhrmaster
At the end of this year’s open enrollment period for insurance coverage through the Affordable Care Act (ACA) Marketplace, signups in Montana decreased by about 6%, on par with the nationwide decline, according to preliminary data from the Centers for Medicare and Medicaid Services (CMS).
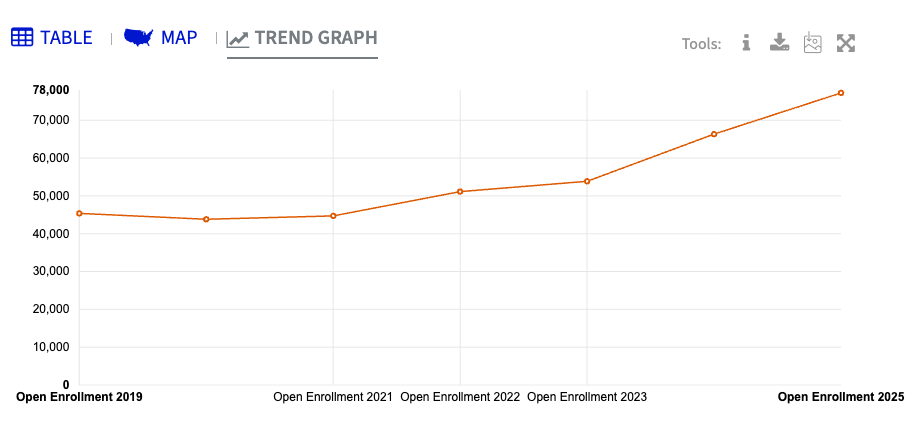
Last year, 77,221 Montanans opted into federal healthcare exchange plans, with 89% of those receiving enhanced premium tax credits that expired in December. This year, 72,402 Montanans enrolled in plans through Healthcare.gov, marking the first time state numbers have gone down since 2020.
Nationwide enrollment also dropped for the first time since 2020. Signups for states using Healthcare.gov are down 5% and state-based plans are down 4%.
The preliminary numbers come before ratepayers “effectuate” their enrollment by paying premiums for their first month, Montana’s Commissioner of Securities and Insurance James Brown said in a press release on Feb. 2. The national open enrollment period ended on Jan. 15 with CMS publishing a national open enrollment snapshot on Jan. 28.
“This preliminary report indicates that Marketplace plan selections in Montana are down by about 6 percent compared to last year,” Brown said. “Our office will continue monitoring enrollment as final numbers are confirmed, and we remain focused on making sure Montanans understand their coverage options and know where to get help.”
National marketplace numbers jumped after the introduction of the enhanced credits in 2021, with enrollment more than doubling from 11 million to over 24 million people. Montana saw a similar spike in enrollment from 2021 to 2025, though factors of in-migration and shifting eligibility also likely play a role, University of Montana health economics Professor Katrina Mullan said.
New marketplace enrollees are generally required to submit their first premium payment within 30 days from their coverage effective date. Meanwhile, returning ratepayers often have a three-month grace period – until March 31 – to catch up on any missed payments before they are booted off a marketplace plan.
The preliminary data combines those who selected healthcare plans and those with marketplace plans last year who were automatically re-enrolled. It remains to be seen whether enrollment numbers will drop again when higher premiums as a result of the expired enhanced tax credits begin to hit ratepayers’ pocketbooks. Increases could range from 56% to 231% depending on individual demographics, according to estimates by health policy research nonprofit KFF.
“There’s still a question mark about people who were [automatically] reenrolled, whether when they see their premiums when they get their bills, they’ll actually pay those higher premiums or whether they’ll drop out at that point,” Mullan said.
CMS usually publishes final enrollment data in July, according to KFF.
Brown encourages those with health insurance questions to reach out to the commissioner’s office by calling 406-444-2040 or visiting their website at csimt.gov.